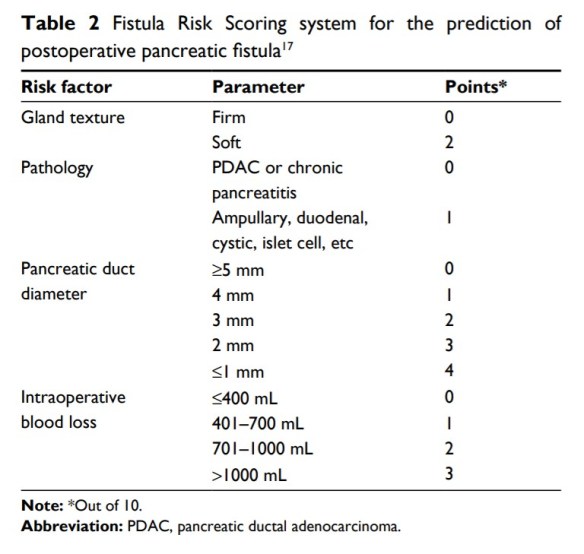
This week’s discussion included risk scoring and management of postoperative pancreatic fistula.
Nahm CB, Connor SJ, Samra JS, Mittal A. Postoperative pancreatic fistula: a
review of traditional and emerging concepts. Clin Exp Gastroenterol. 2018 Mar
15;11:105-118.
Prediction: “Biochemical markers of POP after pancreatic resection are evident from the first postoperative day. These include serum amylase and lipase, and urinary trypsinogen-2. In an observational study of 61 patients undergoing pancreatic resection, the presence of POP on the first postoperative day as determined by these markers was found to be a strong predictor of the development of POPF (OR 17.81, 95% CI 2.17–145.9) [128]
Histological assessment of the pancreatic neck margin to determine the acinar cell density has also been shown to strongly predict the development of POPF (AUROC 0.744, p=0.003). [128] This may be determined in the intraoperative phase at the time of frozen section. Future studies in larger cohorts are required to validate this finding, and to assess whether the acinar cell density may be a more accurate and quantitative way to characterize the remnant gland than simply assessing glandular “texture.”” (pg. 114)
Smits FJ, van Santvoort HC, Besselink MG, et al. Management of Severe Pancreatic Fistula After Pancreatoduodenectomy. JAMA Surg. 2017 Jun 1;152(6):540-548.
Results: “Of the 309 patients included in the analysis, 209 (67.6%) were men, and mean (SD) age was 64.6 (10.1) years. Overall in-hospital mortality was 17.8% (55 patients): 227 patients (73.5%) underwent primary catheter drainage and 82 patients (26.5%) underwent primary relaparotomy. Primary catheter drainage was successful (ie, survival without relaparotomy) in 175 patients (77.1%). With propensity score matching, 64 patients undergoing primary relaparotomy were matched to 64 patients undergoing primary catheter drainage. Mortality was lower after catheter drainage (14.1% vs 35.9%; P = .007; risk ratio, 0.39; 95% CI, 0.20-0.76). The rate of new-onset single-organ failure (4.7% vs 20.3%; P = .007; risk ratio, 0.15; 95% CI, 0.03-0.60) and new-onset multiple-organ failure (15.6% vs 39.1%; P = .008; risk ratio, 0.40; 95% CI, 0.20-0.77) were also lower after primary catheter drainage.”
Further reading:
Bouras AF, Marin H, Bouzid C, et al. Pancreas-preserving management in reinterventions for severe pancreatic fistula after pancreatoduodenectomy: a systematic review. Langenbecks Arch Surg. 2016 Mar;401(2):141-9. Full-text for Emory users.
Ke Z, Cui J, Hu N, Yang Z, et al. Risk factors for postoperative pancreatic fistula: Analysis of 170 consecutive cases of pancreaticoduodenectomy based on the updated ISGPS classification and grading system.Medicine (Baltimore). 2018 Aug;97(35):e12151.
Zhou YM, Zhou X, Wan T, et al. An evidence-based approach to the surgical interventions for severe pancreatic fistula after pancreatoduodenectomy.Surgeon. 2018 Apr;16(2):119-124. Full-text for Emory users.
