Lau C, et al. A retrospective study to determine the cefepime-induced neurotoxicity threshold in hospitalized patients. J Antimicrob Chemother. 2020 Mar 1;75(3):718-725.
Full-text for Emory users.
Results: In total, 206 patients were administered 259 courses of cefepime, with an overall CIN incidence of 6% (16/259 courses). A total of 64 courses had a cefepime trough concentration measured (24.7%). A cefepime trough concentration of 36 mg/L provided the best differentiation between patients who experienced neurotoxicity and those who did not. No other patient covariates were identified to be significantly associated with neurotoxicity occurring.
Conclusions: A cefepime trough plasma concentration ≥36 mg/L appears to be the most sensitive and specific cut-off to predict CIN occurring. No patient factors were associated with the development of CIN when accounting for cefepime trough plasma concentrations.
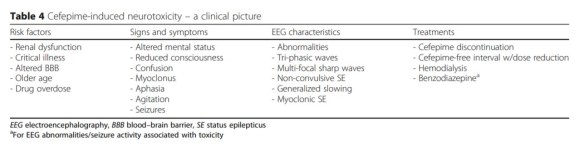
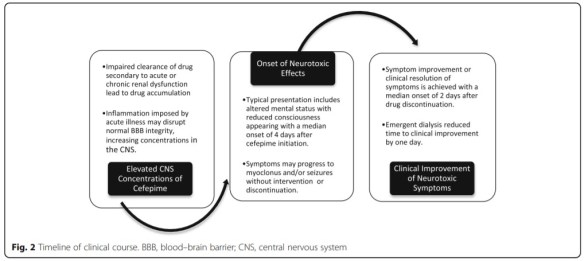
Payne LE, et al. Cefepime-induced neurotoxicity: a systematic review. Crit Care. 2017 Nov 14;21(1):276.
Li HT, et al. Clinical, Electroencephalographic Features and Prognostic Factors of Cefepime-Induced Neurotoxicity: A Retrospective Study. Neurocrit Care. 2019 Oct;31(2): 329-337.
Full-text for Emory users.
A total of 42 CIN patients were identified, including 25 patients from wards and 17 from intensive care units; their mean age was 75.8 ± 11.8 years. Twenty-one patients (50%) had chronic kidney disease, and 18 (43%) had acute kidney injury. Among these patients, 32 (76%) received appropriate cefepime dose adjustment. Three patients had a normal renal function at the time of CIN onset. The logistic regression model suggested that maintenance hemodialysis and longer duration of cefepime use were independently associated with the development of CIN, with odds ratios of 3.8 and 1.2, respectively. NCSE was frequently noted in the CIN patients (64%). Generalized periodic discharge with or without triphasic morphology was the most common EEG pattern (38%), followed by generalized rhythmic delta activity and generalized spike-and-waves. AEDs were administered to 86% of the patients. A total of 17 patients (40%) did not survive to hospital discharge. Adequate cefepime dose adjustment and early cefepime discontinuation led to a better prognosis.
More PubMed results on cefepime-induced neurotoxicity .
