Hornor MA, Duane TM, Ehlers AP, et al. ACS Guidelines for the Perioperative Management of Antithrombotic Medication. J Am Coll Surg. 2018 Nov;227(5):521-536.e1.
Full-text for Emory users.

Filipescu DC, et al. Perioperative management of antiplatelet therapy in noncardiac surgery. Curr Opin Anaesthesiol. 2020 Jun;33(3):454-462.
Full-text for Emory users.
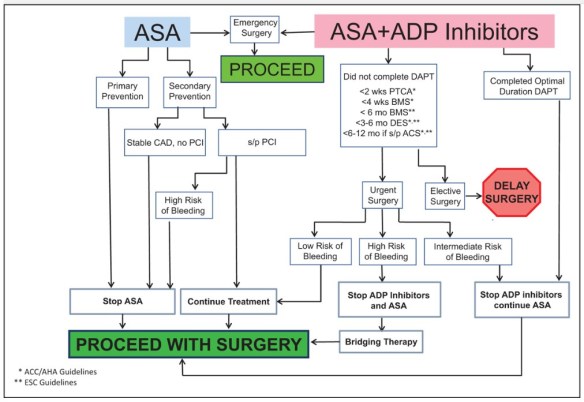 FIGURE 1. Algorithm for perioperative management of antiplatelet therapy in patients with coronary artery disease. ACS, acute coronary syndrome; ADP, adenosine diphosphate; ASA, aspirin; BMS, bare-metal stents; CAD, coronary artery disease; DAPT, dual antiplatelet therapy; DES, drug-eluting stent; PCI, percutaneous coronary intervention; PTCA, percutaneous transluminal coronary angioplasty. Adapted with permission [9].
FIGURE 1. Algorithm for perioperative management of antiplatelet therapy in patients with coronary artery disease. ACS, acute coronary syndrome; ADP, adenosine diphosphate; ASA, aspirin; BMS, bare-metal stents; CAD, coronary artery disease; DAPT, dual antiplatelet therapy; DES, drug-eluting stent; PCI, percutaneous coronary intervention; PTCA, percutaneous transluminal coronary angioplasty. Adapted with permission [9].
Douketis JD, et al. Perioperative management of antithrombotic therapy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012 Feb;141(2 Suppl):e326S-e350S. Erratum in: Chest. 2012 Apr;141(4):1129.
- 2.1. In patients who require temporary interruption of a VKA before surgery, we recommend stopping VKAs approximately 5 days before surgery instead of stopping VKAs a shorter time before surgery (Grade 1B) .
- 2.2. In patients who require temporary interruption of a VKA before surgery, we recommend resuming VKAs approximately 12 to 24 h after surgery (evening of or next morning) and when there is adequate hemostasis instead of later resumption of VKAs (Grade 2C) .
- 2.4. In patients with a mechanical heart valve, atrial fibrillation, or VTE at high risk for thromboembolism, we suggest bridging anticoagulation instead of no bridging during interruption of VKA therapy (Grade 2C).
- 3.5. In patients at moderate to high risk for cardiovascular events who are receiving ASA therapy and require noncardiac surgery, we suggest continuing ASA around the time of surgery instead of stopping ASA 7 to 10 days before surgery (Grade 2C).
- In patients at low risk for cardiovascular events who are receiving ASA therapy, we suggest stopping ASA 7 to 10 days before surgery instead of continuation of ASA (Grade 2C).
Gotoh S, et al. Management of Antithrombotic Agents During Surgery or Other Kinds of Medical Procedures With Bleeding: The MARK Study. J Am Heart Assoc. 2020 Mar 3;9(5):e012774.
The participants were 9700 patients who received oral antithrombotic agents and underwent scheduled medical procedures with bleeding at 59 National Hospital Organization institutions in Japan.
Primary outcomes were thromboembolic events, bleeding events, and death within 2 weeks before and 4 weeks after the procedures. We investigated the relationships between each outcome and patient demographics, comorbidities, type of procedure, and management of antithrombotic therapy. With respect to the periprocedural management of antithrombotic agents, 3551 patients continued oral antithrombotic agents (36.6%, continuation group) and 6149 patients discontinued them (63.4%, discontinuation group).
The incidence of any thromboembolic event (1.7% versus 0.6%, P<0.001), major bleeding (7.6% versus 0.4%, P<0.001), and death (0.8% versus 0.4%, P<0.001) was all greater in the discontinuation group than the continuation group. In multivariate analysis, even after adjusting for confounding factors, discontinuation of anticoagulant agents was significantly associated with higher risk for both thromboembolic events (odds ratio: 4.55; 95% CI, 1.67–12.4; P=0.003) and major bleeding (odds ratio: 11.1; 95% CI, 2.03–60.3; P=0.006) in procedures with low bleeding risk.
In contrast, heparin bridging therapy was significantly associated with higher risk for both thromboembolic events (odds ratio: 2.03; 95% CI, 1.28–3.22; P=0.003) and major bleeding (odds ratio: 1.36; 95% CI, 1.10–1.68; P=0.005) in procedures with high bleeding risk.
More PubMed results for perioperative management of antiplatelet therapy.

Pingback: Periprocedural bridging anticoagulation | Surgical Focus
Pingback: Digest for July 4-10, 2022 | Surgical Focus