de Jonge SW, et al. Systematic Review and Meta-Analysis of Randomized Controlled Trials Evaluating Prophylactic Intra-Operative Wound Irrigation for the Prevention of Surgical Site Infections. Surg Infect (Larchmt). 2017 May/Jun;18(4):508-519. Full-text for Emory users.
“Although recommendations from existing guidelines are conflicting [9,10] and recent well-designed RCTs are lacking, as many as 97% of surgeons irrigate wounds in an effort to reduce the risk of SSI [6,7]. The most commonly used irrigation solution is saline followed by aqueous PVP-I or antibiotic solutions [6,42,43]. The efficacy and clinical safety of irrigation with these solutions has been the subject of debate [11, 44]. Various concentrations of PVP-I are effective rapidly against a broad spectrum of pathogens, methicillin-resistant S. aureus (MRSA) included [45,46]. However, some in vitro studies [47-49] have reported a negative effect of PVP-I on tissue regeneration, and older case studies describe serum iodine toxicity as a result of irrigation [50-52]. However, these adverse effects could not be substantiated in clinical trials [29-35;41].” (p. 515)

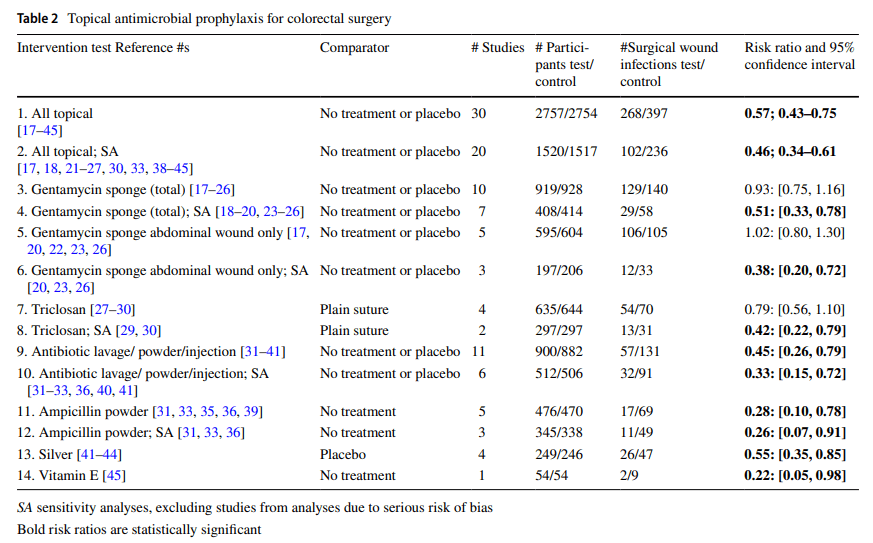
Nelson RL, et al. Topical antimicrobial prophylaxis in colorectal surgery for the prevention of surgical wound infection: a systematic review and meta-analysis. Tech Coloproctol. 2018 Aug;22(8):573-587. Erratum in: Tech Coloproctol. 2019 Apr 1. Full-text for Emory users.
“Antibiotic lavage showed a significant decrease in SSI (RR 0.45, 95% CI 0.26–0.79; low-quality evidence) which increased after sensitivity analysis (RR 0.33, 95% CI 0.15–0.72; moderate-quality evidence).” (p. 573)
Edmiston CE Jr, et al. Reducing the risk of surgical site infections: does chlorhexidine gluconate provide a risk reduction benefit? Am J Infect Control. 2013 May;41(5 Suppl):S49-55.
“A new focus for the use of CHG in surgical patients involves irrigation of the wound prior to closure with 0.05% CHG followed by saline rinse. Recent laboratory studies suggest that, following a 1-minute exposure, 0.05% CHG produces a >5-log reduction against selective health care-associated pathogens and reduces microbial adherence to the surface of implantable biomedical devices. General, orthopedic, cardiothoracic, and obstetrical surgical studies have documented the safety of selective CHG formulations in elective surgical procedures.” (p. S49)

“Mechanistically, most antimicrobials agents are effective against microorganisms when drug exposure occurs during their logarithmic growth phase. Therefore, the process of antibiotic-lavage or irrigation does not realistically afford sufficient contact time to efficiently kill or inhibit bacterial growth within the peritoneal cavity.” (p. S52)
Norman G, et al. Intracavity lavage and wound irrigation for prevention of surgical site infection. Cochrane Database Syst Rev. 2017 Oct 30;10(10):CD012234.
Authors’ conclusions: The evidence base for intracavity lavage and wound irrigation is generally of low certainty. Therefore where we identified a possible difference in the incidence of SSI (in comparisons of antibacterial and non-antibacterial interventions, and pulsatile versus standard methods) these should be considered in the context of uncertainty, particularly given the possibility of publication bias for the comparison of antibacterial and non-antibacterial interventions.
More PubMed results on the effectiveness of surgical irrigation on SSI rates.
