“A surgical site infection (SSI) is defined as an infection of the incision (superficial SSI), the
tissue below the incision (deep SSI), or within the abdominal cavity (organ space SSI). SSI
accounts for more than 20% of all health care-associated infections and is the most common
infection after surgery, affecting an estimated 300,000 patients annually. Compared with
other surgical subspecialties, patients undergoing colorectal surgery are at the highest risk
for developing an SSI with an estimated incidence of 5% to 30%. Patients undergoing
emergency colorectal surgery with colon perforation have an SSI incidence as high as 80%.”
TABLE 2.
Summary and strength of GRADE recommendations for preventing SSIs
| Summary | Recommendation strength | GRADE quality of evidence | |
|---|---|---|---|
| 1 | Implementing an SSI bundle for patients undergoing colorectal surgery can decrease the incidence of SSI | Strong | Moderate |
| 2 | Oral antibiotics in combination with mechanical bowel preparation have been shown to decrease the incidence of SSI after elective colorectal resection | Strong | Moderate |
| 3 | In circumstances where a mechanical bowel preparation is contraindicated or otherwise omitted, preoperative oral antibiotic preparation alone can reduce the incidence of SSI | Conditional | Moderate |
| 4 | Showering with chlorhexidine before colorectal surgery does not significantly impact SSI rates | Strong | Moderate |
| 5 | Smoking cessation before surgery may be recommended to reduce the risk of SSI | Conditional | Moderate |
| 6 | On the day of colorectal surgery, patients should have their hair removed from the surgical site using a clipper or not removed at all. Shaving with a razor before surgery is discouraged | Strong | Moderate |
| 7 | Patients undergoing colorectal resection should have parenteral antibiotics administered within 60 min of incision. Dosing and redosing should be based on the pharmacokinetic profile of the antibiotic | Strong | Low |
| 8 | Patients who report a penicillin allergy may be evaluated for having true hypersensitivity and high-risk reactions to penicillin. Delabeling a penicillin-allergic patient can facilitate the appropriate use of a preoperative prophylactic beta-lactam antibiotic and improve outcomes | Conditional | Low |
| 9 | For most clean and clean-contaminated cases, prophylactic parenteral antibiotics should be limited to the initial 24 h postoperatively | Strong | Moderate |
| 10 | Cleansing the surgical site with chlorhexidine–alcohol-based preparation is typically recommended for patients undergoing colorectal surgery | Strong | Moderate |
| 11 | Hyperglycemia on the day of surgery and in the immediate postoperative period may increase the risk of SSI after elective colorectal resection | Conditional | Moderate |
| 12 | Maintaining intraoperative normothermia may decrease the incidence of SSI in patients undergoing colorectal surgery | Conditional | Low |
| 13 | High-fractionated oxygen is not routinely recommended to prevent SSI | Conditional | Moderate |
| 14 | Wound protectors can decrease the incidence of SSI after colorectal surgery | Strong | High |
| 15 | Minimally invasive colorectal surgery can decrease the incidence of SSI compared to open surgery | Strong | High |
| 16 | Topical antimicrobial agents applied to the surgical incision are not recommended | Strong | Low |
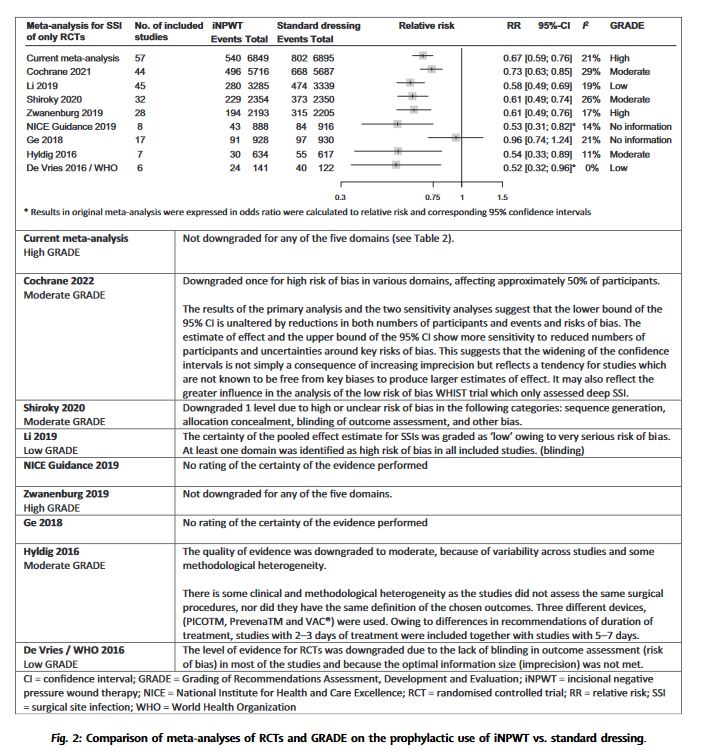
| 17 | NPWT for primarily closed incisions may decrease the incidence of SSI | Conditional | Moderate |
| 18 | Advanced silver or antimicrobial dressings are not routinely recommended for clean or clean-contaminated wounds after colorectal surgery | Conditional | Moderate |
GRADE = Grading of Recommendations, Assessments, Development, and Evaluation; NPWT = Negative pressure wound therapy; SSI = surgical site infection.
Continue reading