One discussion this week involved the comparison of simultaneous and staged resections of colorectal cancer and synchronous colorectal liver metastases (SCRLM).
Reference: Reddy SK, et al. Simultaneous resections of colorectal cancer and synchronous liver metastases: a multi-institutional analysis. Annals of Surgical Oncology. 2007 Dec;14(12):3481-3491. doi:10.1245/s10434-007-9522-5
Summary: In a retrospective study of 610 patients at three institutions between 1985 and 2006, the authors compared postoperative morbidity and mortality after simultaneous and staged resections of colorectal cancer and SCRLM.
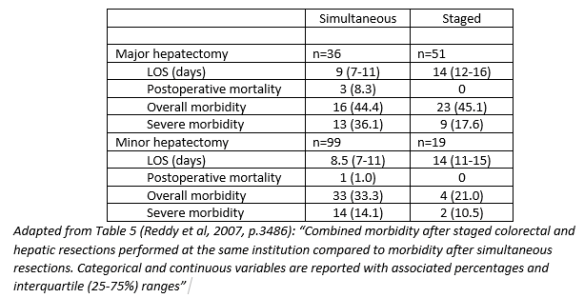
Minor hepatic resection – Simultaneous patients had shorter lengths of stay with no differences in morbidity or mortality. Simultaneous colorectal resection and minor hepatectomy can be done safely and with no differences in mortality, severe morbidity, hepatic related morbidity, intraoperative blood loss, or frequency of blood transfusion compared to minor hepatic resection alone (p.3486).
Major hepatic resection – Univariate analysis showed that severe postoperative morbidity was possibly associated with major hepatic resection and intraoperative red blood cell transfusion. Increased risks of mortality, overall morbidity, severe morbidity, and positive hepatic resection margins are found in performing simultaneous major hepatic and colorectal resections compared to major hepatectomy alone. In fact, major hepatectomy involved a more than threefold risk of severe morbidity among simultaneous patients.
The authors clearly state when they do not recommend simultaneous colorectal and hepatic resections:
- Do not resect liver metastases found on exploration during emergent colorectal cancer resection for perforation, obstruction, or bleeding
- In cases of perforation because of high likelihood for peritoneal carcinomatosis
- When the odds of postoperative hepatic insufficiency are high (cirrhotics or long-standing chronic liver disease)
- Patients in whom the future liver remnant is likely to provide borderline or insufficient hepatic function
- In the presence of extrahepatic disease.
(p.3489)

Pingback: Simultaneous resection of primary colorectal cancer and synchronous liver metastases | Surgical Focus