One discussion this week involved neurological outcomes following ECMO resuscitation.
Reference: Ryu JA, et al. Predictors of neurological outcomes after successful extracorporeal cardiopulmonary resuscitation. BMC Anesthesiology. 2015 Mar 8;15:26. doi: 10.1186/s12871-015-0002-3
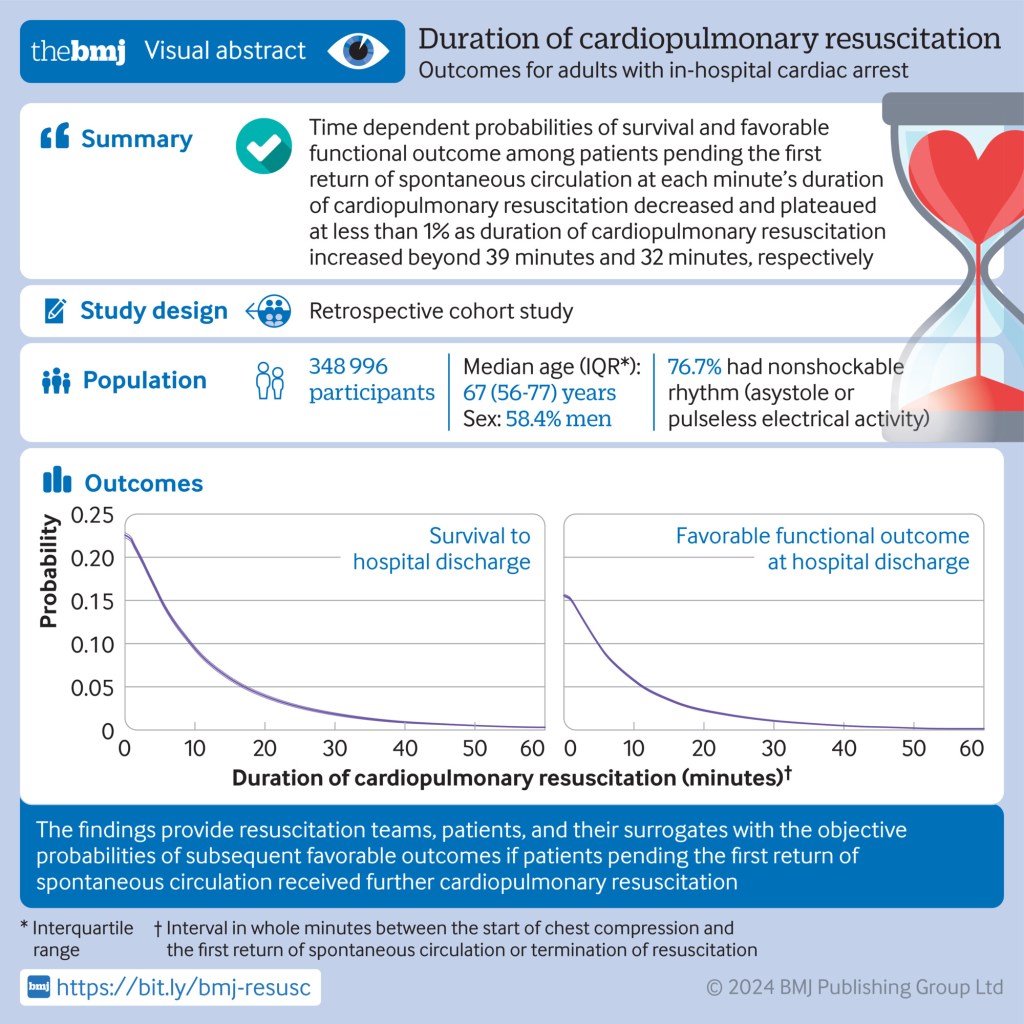
Summary: Extracorporeal membrane oxygenation (ECMO) is a useful intervention for refractory cardiogenic shock and respiratory failure. Because ECMO implementation can rapidly normalize circulation in patients under cardiac arrest, it has been used to assist cardiopulmonary resuscitation (CPR). Using traditional chest compression is less effective than using ECMO with CPR (known as extracorporeal CPR or ECPR). ECPR can achieve more effective recovery of spontaneous circulation (ROSC) than conventional CPR.
Since the brain is the organ most vulnerable to hypoxia and inadequate perfusion, ECPR can result in severe neurologic deficits if ECMO is not performed promptly. In addition to delay, several factors may lead to poor neurological outcomes after ECPR. Achieving good neurological outcomes and successful resuscitation are important, so the authors investigated predictors of favorable neurological outcomes rather than survival after ECPR.
The study’s primary endpoint was neurological outcome at hospital discharge, assessed with the Glasgow-Pittsburgh Cerebral Performance Categories (CPC) scale (1 to 5, as shown in Table ). CPC 1 and 2 were classified as good neurological outcomes. CPC 3, 4, and 5 were considered poor neurological outcomes.
Of 115 patients, 68 (59%) had good neurological outcomes but 47 (41%) did not (Figure ). Therapeutic hypothermia was performed in 10 patients (5%). Mean duration of ECMO support was 47.5 (range 18.5–101) hours. Total length of stay in intensive care unit (ICU) was 11 (range 7–22.5) days and 24 patients died from brain death.
Univariate analysis showed no differences between the good and poor neurological outcome groups for age, comorbidities, bystander CPR, therapeutic hypothermia, total bilirubin, creatinine, 24-hour lactic acid clearance, ROSC before ECMO, or ROSC time (Table ).
Multivariate analysis revealed neurological outcomes were affected by hemoglobin level, serum lactic acid before ECMO insertion, and interval from cardiac arrest to ECMO (Figure ). However, age, gender, cardiac arrest out of the hospital, hemoglobin level after ECMO, acute coronary syndrome, initial shockable rhythm, and CPR duration were not independent predictors of neurological outcomes (Table ).

 Click to enlarge.
Click to enlarge.