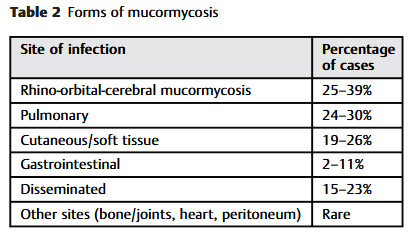
“Mucormycosis is an infection caused by a group of filamentous molds within the orders Mucorales and Entomophthorales. Mucorales occupy environmental niches including soil, decaying vegetable matter, bread, and dust. Infections due to Mucorales may result from inhalation of spores into the respiratory tract, ingestion of contaminated foods, or
inoculation of disrupted skin or wounds. In developed countries, mucormycosis occurs primarily in severely immunocompromised hosts. In contrast, in developing countries, a substantial number of cases of mucormycosis occur in patients with poorly controlled diabetes mellitus (DM) or persons who have sustained trauma. Mucormycosis exhibits a marked propensity to invade blood vessels, leading to thrombosis, necrosis, and infarction of tissue, and mortality is high.”