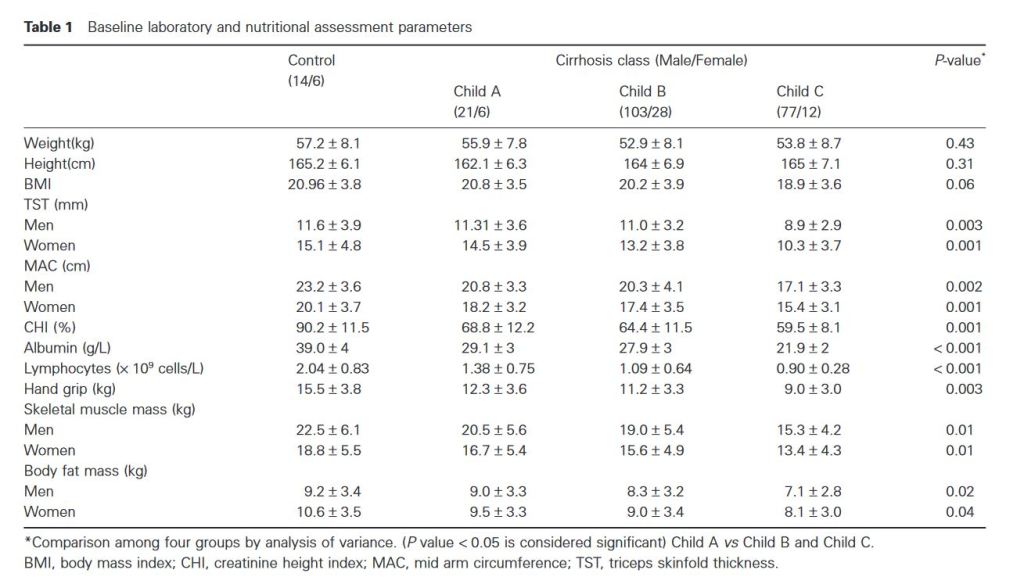
“Prevalence of malnutrition in chronic liver disease ranges between 10% and 100%, depends on severity of liver disease. Prevalence is more in patients with alcoholic cirrhosis compared to nonalcoholic cirrhotics. 3 Malnutrition is seen in all clinical stages but is easier to detect in advanced stages of liver cirrhosis. Many patients have subtle changes such as fat soluble vitamin deficiency, anemia from iron, folate or pyridoxine deficiency, altered cell-mediated immune functions and minimal loss of muscle mass, while patients with end-stage liver disease have muscle wasting, decreased fat stores, and cachexia.”