“Percutaneous endoscopic gastrostomy (PEG) tube placement is a commonly performed procedure in trauma patients.Since the establishment of the acute care surgery (ACS)
model, the role of ACS in PEG tube placement in many institutions has expanded. The incidence of PEG tube complications has been under-reported in the literature and varies
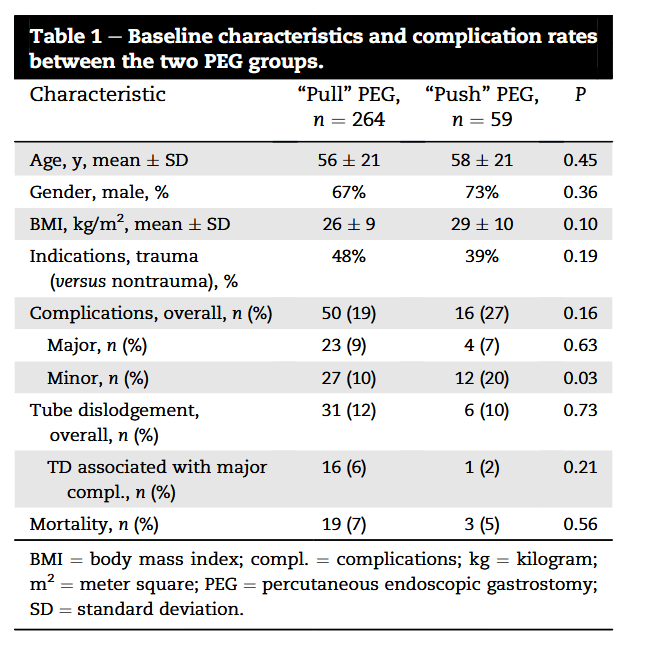
widely among the patient populations studied and the definition of complications utilized. Major and minor complications may range from 3% to 26%. Our institution, under an ACS model, has previously reported an overall 25% complication rate with 10% major and 14% minor complications associated with pull PEG.”