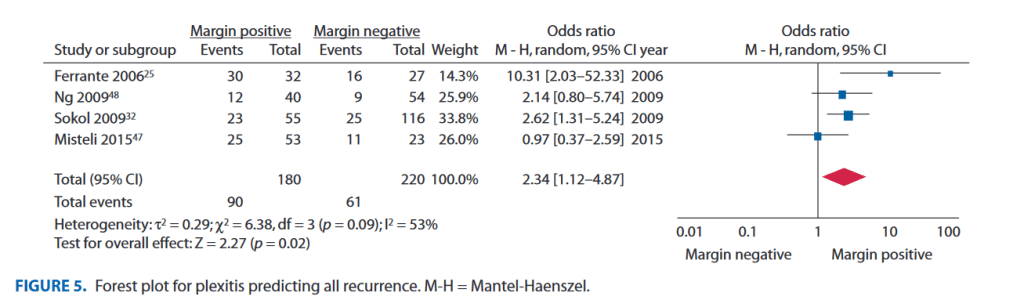
“The presence of involved histological margins at the time of index resection in Crohn’s disease is associated with recurrence, and plexitis shows promise as a marker of more aggressive disease. Further studies with homogeneity of histopathological and recurrence reporting are required.“”The presence of involved histological margins at the time of index resection in Crohn’s disease is associated with recurrence, and plexitis shows promise as a marker of more aggressive disease. Further studies with homogeneity of histopathological and recurrence reporting are required.“