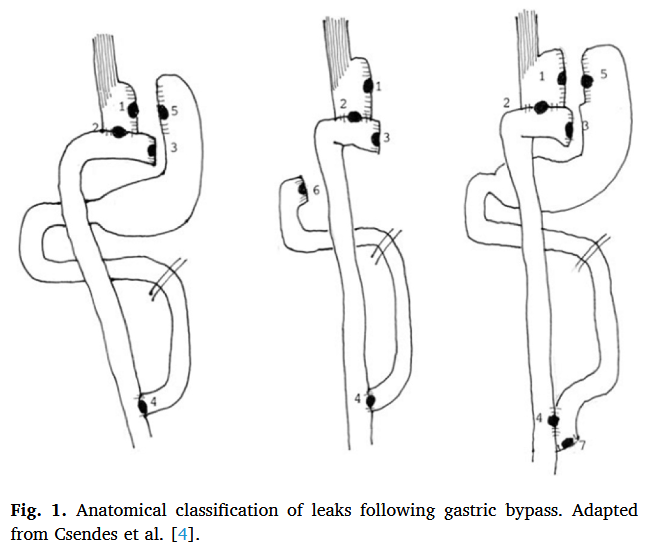
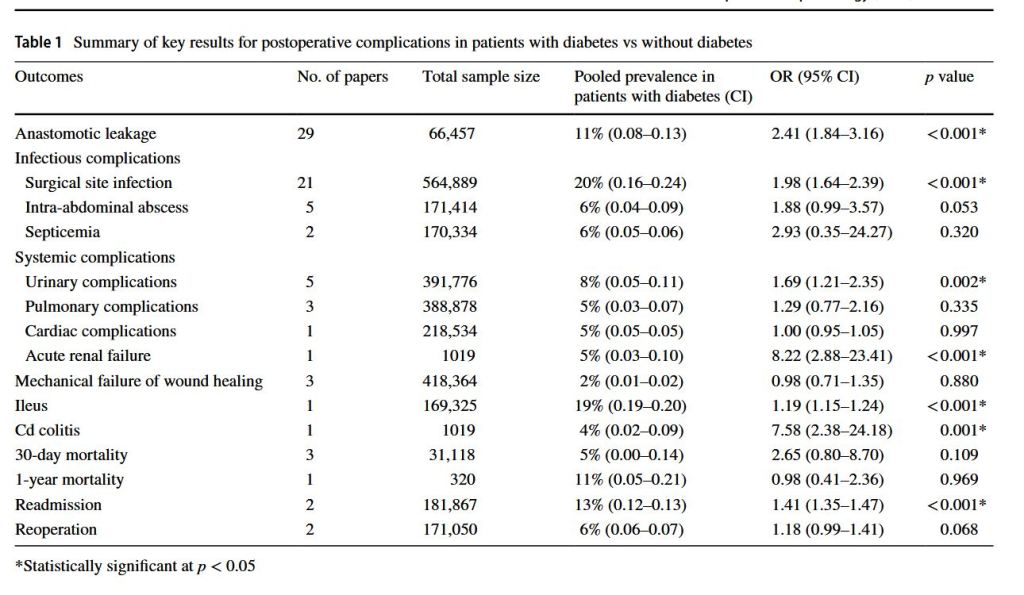
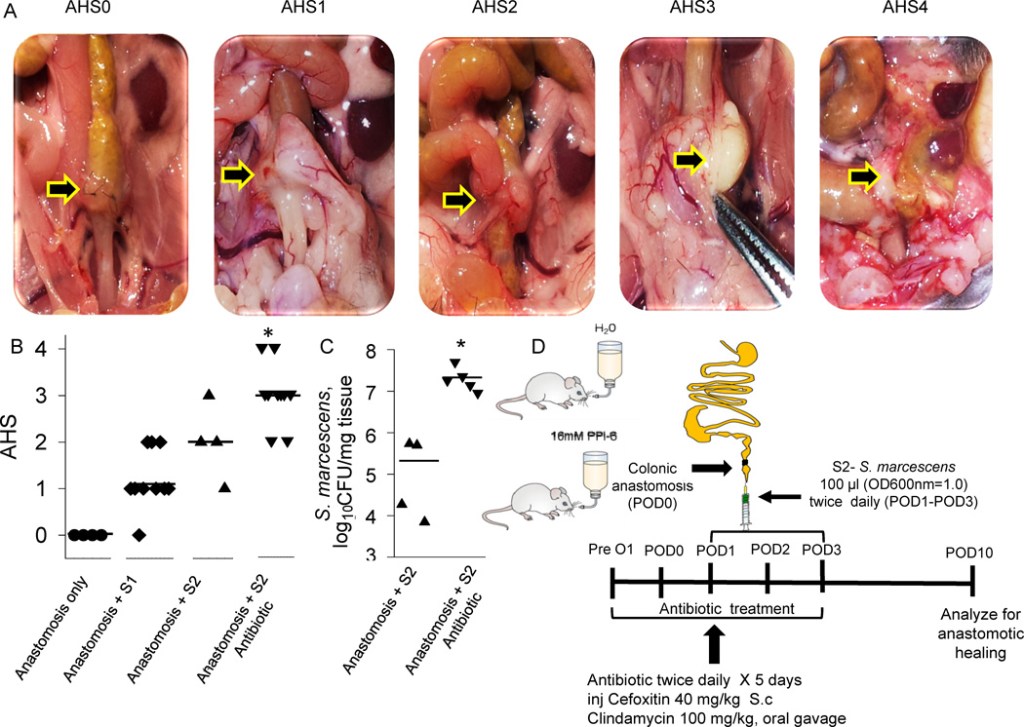
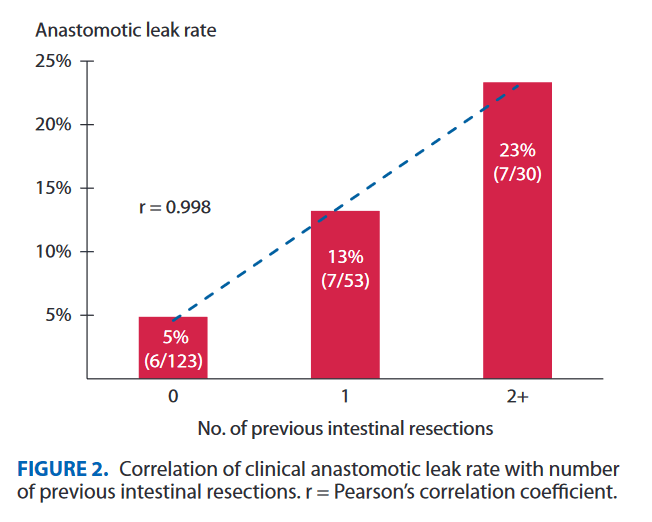
“Leaks and fistulas are among the most feared complications of bariatric surgery. Variable in presentation, acuity, and severity, these often require multimodal and multispecialty management strategies for optimal outcomes. Recent advancements in the realm of endoscopic therapies have made these integral to the treatment algorithm of post-operative leaks and fistulas. In this review, we will discuss the epidemiology, pathophysiology and classification of post-bariatric surgery defects and provide an in-depth assessment of current management strategies, with a focus on endoscopic therapies.”