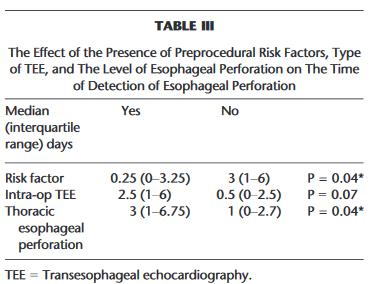
“Transesophageal echocardiography (TEE) is a commonly performed procedure, either in an
intra-operative setting of a cardiac surgical procedure or a nonoperative setting, such as to evaluate for an intracardiac thrombi.”

“Transesophageal echocardiography (TEE) is a commonly performed procedure, either in an
intra-operative setting of a cardiac surgical procedure or a nonoperative setting, such as to evaluate for an intracardiac thrombi.”

“Mesh properties and position within the abdominal wall are the primary determinants in the ability to salvage mesh in the event of PMI. Mesh placed in an intraperitoneal position is rarely salvageable. Similarly, microporous, multifilament, and composite mesh constructs required complete mesh removal in most cases. However, macroporous, monofilament PP mesh in an extraperitoneal position can be salvaged in 72.2% of cases, positively impacting both the need for reoperation for mesh removal and subsequent hernia
recurrence.” (Warren)
“Surgical site infections (SSI) are common complications after open ventral hernia repair (OVHR), potentially requiring further intervention. Incidence of surgical site occurrence was significantly lower after G 1 C irrigation (Grp 1, 28.1%; Grp 2, 35.4%; Grp 3, 19.7%; P < 0.001). Incidence of SSI was significantly lower after G 1 C irrigation, but not G
alone (Grp 1, 16.5%; Grp 2, 15.2%; and Grp 3, 5.4%; P < 0.001). Multivariate logistic regression demonstrated significantly increased SSI with contaminated wounds (OR 2.96; 95% confidence interval (CI) 1.39–6.21), dirty wounds (OR 3.84; 95% CI 1.49–9.69), and chronic obstructive pulmonary disease (OR 3.70; 95% CI 2.16–6.38), as expected. Use of G 1 C was an independent predictor of decreased SSI (OR 0.33; 95% CI 0.16–0.67). Irrigation with a combined G 1 C antibiotic irrigation significantly reduces the incidence of surgical site infection after OVHR with mesh.” (Fatula)
“According to our results, a CT scan triggered by clinical suspicion must be considered the first-line procedure to detect a postoperative leak following primary sleeve gastrectomy or Roux-en-Y gastric bypass.”

A multivariate analysis showed the following adverse risk factors for AL: age > 65 years, hemoglobin < 8.0 g/dL and malnourishment. A multivariable model for AL showed a strong optimism-adjusted discrimination (concordance index, 0.675).

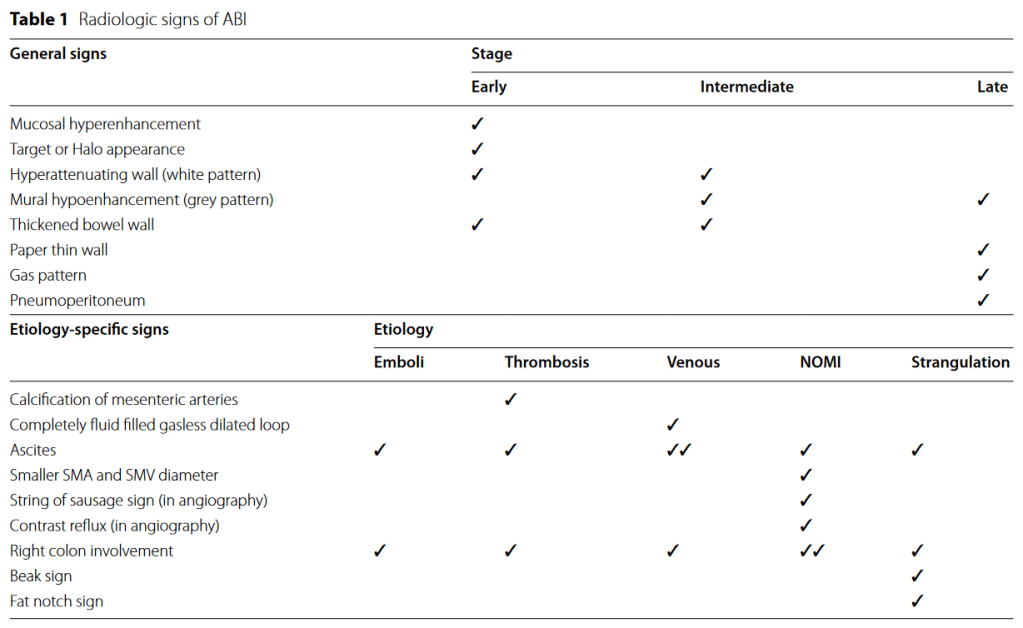
“Acute bowel ischemia (ABI) can be life threatening with high mortality rate. The radiologist plays a central role in the initial diagnosis and preventing progression to irreversible intestinal ischemic injury or bowel necrosis. The most single imaging findings described in the literature are either non-specific or only present in the late stages of ABI, urging the use of a constellation of features to reach a more confident diagnosis”
“The anatomical position of the inferior epigastric artery (IEA) subjects it to risk of injury during abdominal procedures that are close to the artery, such as laparoscopic trocar insertion, insertion of intra-abdominal drains, Tenckhoffâ catheter (peritoneal dialysis catheter) and paracentesis. This article aims to raise the awareness of the anatomical variations of the course of the IEA in relation to abdominal landmarks in order to define a safer zone for laparoscopic ancillary trocar placement. Methods of managing the IEA injury as well as techniques to minimise the risk of injury to the IEA are reviewed and discussed.”
Continue reading