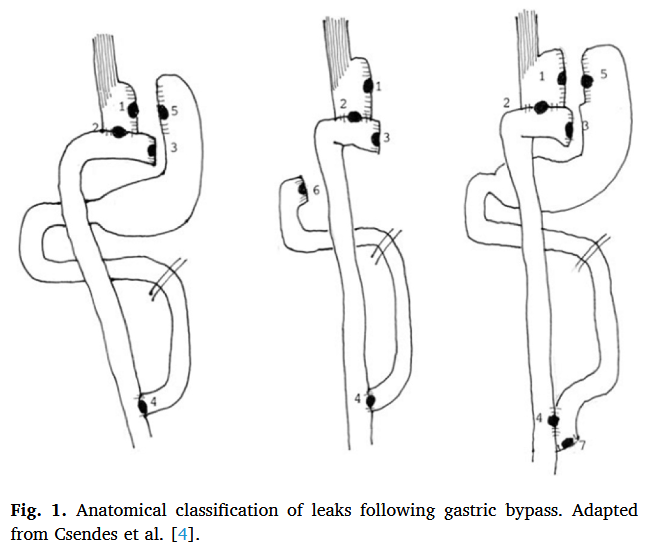
“Higher rates of morbidity and mortality following colonic conduits are reported to be due to be associated with longer operating times and the additional colo-gastric and colo-colic anastomoses. Yet, colonic conduits have the advantages of being longer, acid resistant, and possess an excellent blood supply. No consensus regarding the optimum site of colonic conduit (right vs. left) or placement route (posterior mediastinal, retrosternal or subcutaneous) exists. The operation is usually carried out based on individual surgeons’ preferences and experience, and in the absence of randomised controlled trials, this situation is likely to continue. The aim of this systematic review and meta-analysis was
to determine the optimal site of colonic conduit and route of placement after adult oesophagectomy.”