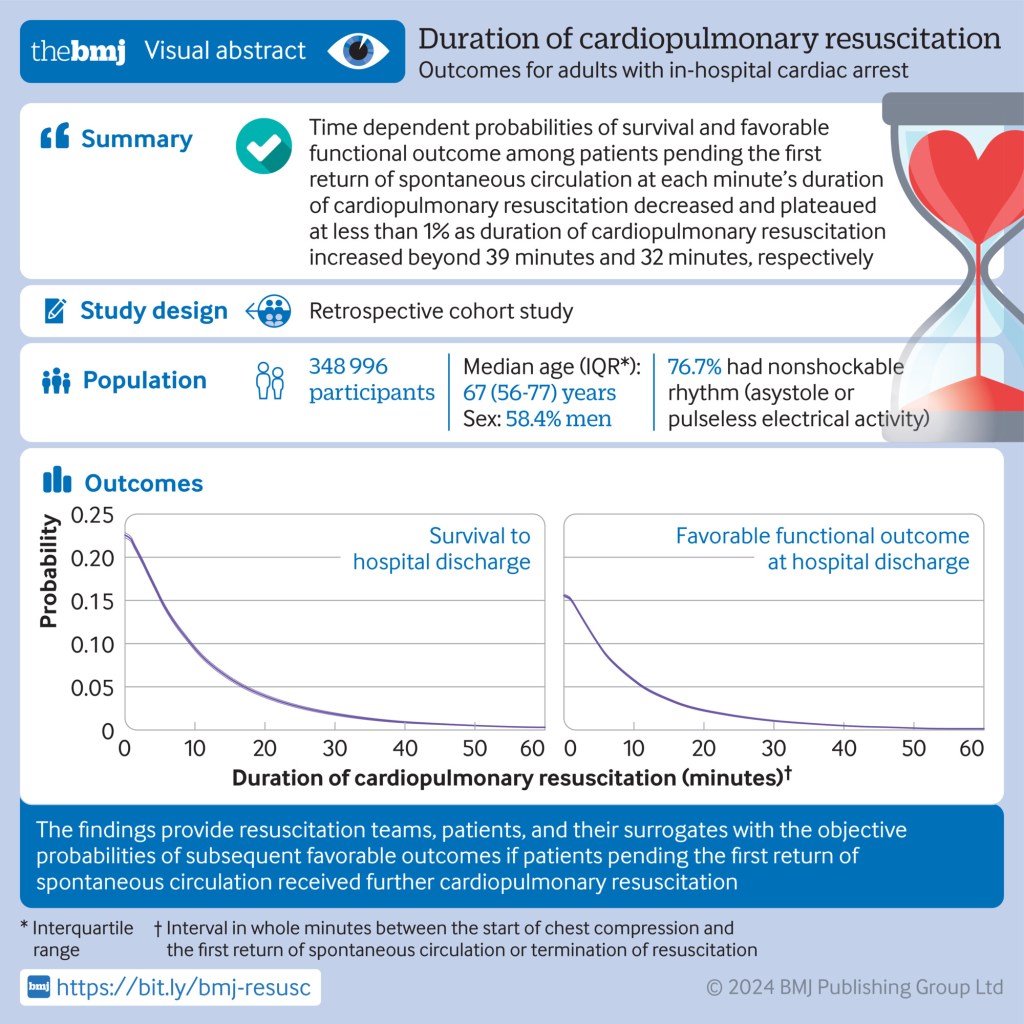
“In-hospital cardiac arrest is an important public health problem, affecting approximately 300 000 adults annually in the United States, with a high mortality rate.1 2 The survival rate after in-hospital cardiac arrest in the US improved from 2000 to 2010 and has remained plateaued after 2010, with approximately 25% of patients surviving to hospital discharge.
Achieving return of spontaneous circulation is the first step toward long term survival and favorable functional recovery. However, for nearly half of patients with in-hospital cardiac arrest, resuscitative efforts are terminated without achievement of return
of spontaneous circulation.”