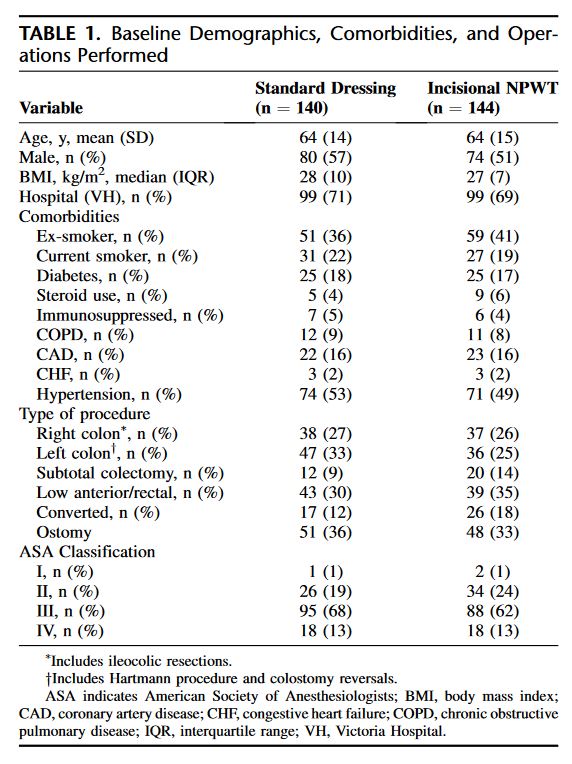
“Surgical site infection (SSI) is one of the most common complications following open colon and rectal surgery. Significant morbidity—secondary to increased length of stay, delay in adjuvant treatments, and psychosocial effects—has been well established in the literature. Further, SSIs confer additional monetary costs to the healthcare system.6 Despite best practice recommendations including prophylactic antibiotics and aseptic technique, SSIs remain common in open colorectal surgery. Rates of SSI in the literature range between 15
and 30%. Increased use of laparoscopy in colorectal surgery has significantly impacted rates of SSI but the uptake of laparoscopy has not been complete as certain patients are not candidates and conversion to open is required in approximately 15% of cases.”