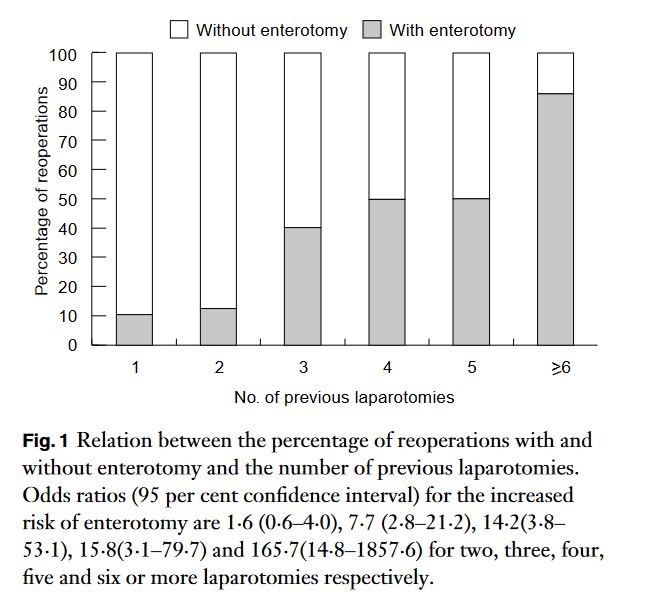
“Postoperative intra-abdominal adhesions are a major concern in modern surgery. Intestinal obstruction is an important and well known clinical consequence of adhesions, resulting in significant morbidity and mortality rates, and high financial costs. Secondary infertility in women and chronic abdominal and pelvic pain are other, frequently cited, adhesion-related problems. Furthermore, intraabdominal adhesions render reoperation dif®cult and may
increase the complication rate of the intended surgical procedure. Prolonged operating time, unfeasibility of the laparoscopic approach and inadvertent enterotomy are known drawbacks of reoperative abdominal surgery, directly related to adhesions.”