“Acute fascia dehiscence (FD) is a threatening complication occurring in 0.4–3.5% of cases after abdominal surgery. Prolonged hospital stay, increased mortality and increased rate of incisional hernias could be following consequences. Several risk factors are controversially discussed. Even though surgical infection is a known, indisputable risk factor, it is still not proven if a special spectrum of pathogens is responsible. In this study, we investigated if a specific spectrum of microbial pathogens is associated with FD.”
Continue readingDiagnosis of Anastomotic Leak
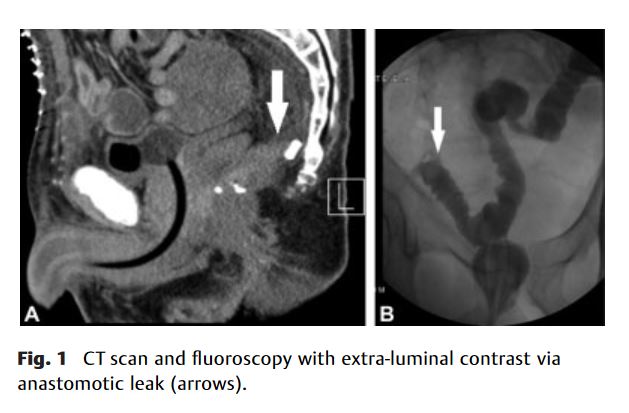
“Anastomotic leaks after colorectal surgery is associated with increased morbidity and
mortality. Understanding the impact of anastomotic leaks and their risk factors can
help the surgeon avoid any modifiable pitfalls. The diagnosis of an anastomotic leak can
be elusive but can be discerned by the patient’s global clinical assessment, adjunctive
laboratory data and radiological assessment. The use of inflammatory markers such as
C-Reactive Protein and Procalcitonin have recently gained traction as harbingers for a
leak. A CT scan and/or a water soluble contrast study can further elucidate the location
and severity of a leak. Further intervention is then individualized on the spectrum of
simple observation with resolution or surgical intervention.”
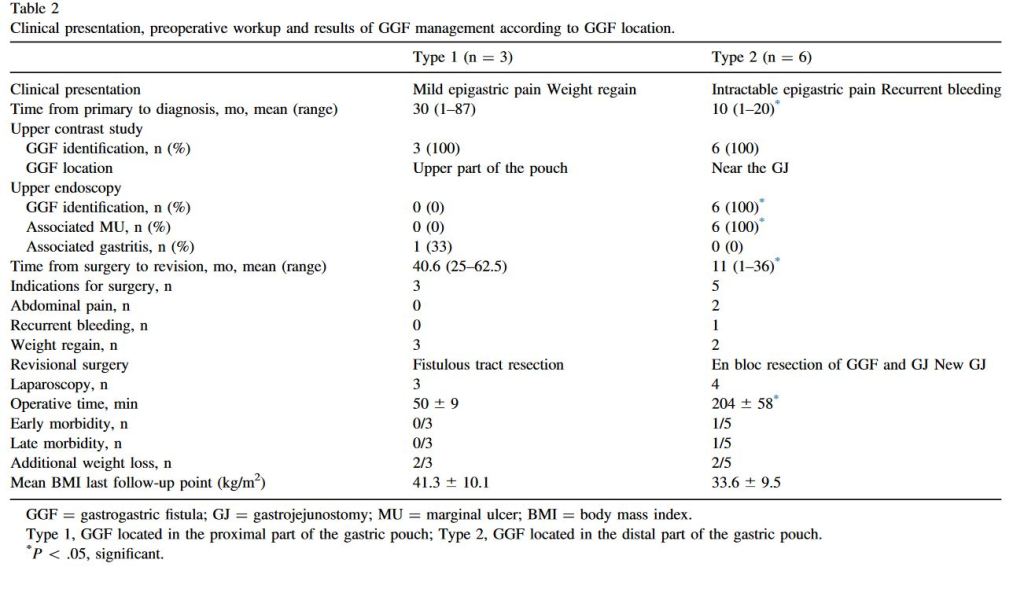
Classification, surgical management and outcomes of patients with gastrogastric fistula after Roux-En-Y gastric bypass
“Gastrogastric fistula (GGF) was a well-described complication after nondivided Roux-en-Y gastric bypass (RYGB), with a documented rate of up to 50%. Gastric transection with isolation of the gastric pouch (divided RYGB) reduces but does not eliminate this complication, which still occurs with a reported incidence ranging from 0% to 6%. Weight regain, epigastric pain, and marginal ulcer (MU) are the most common symptoms. Some GGF can be managed conservatively or by endoscopic approach, but surgery remains the standard of care.”
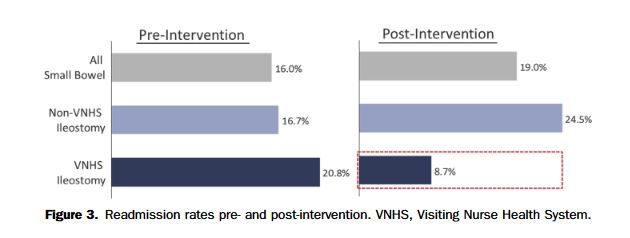
Decreasing Hospital Readmission in Ileostomy Patients
“Nearly 30% of patients with newly formed ileostomies require hospital readmission from severe dehydration or associated complications. This contributes to significant morbidity and rising healthcare costs associated with this procedure. The aim of this study was to design and pilot a novel program to decrease readmissions in this patient population.”
“Implementation of a novel program reduced the 30-day readmission rate by 58% and cost of readmissions per patient by >80% in a high risk for readmission patient population with newly created ileostomies. Future efforts will expand this program to a greater number of patients, both institutionally and systemically, to reduce the readmission-rate and healthcare
costs for this high-risk patient population.”
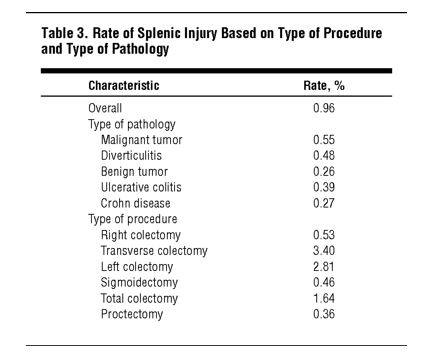
Predictive factors of splenic injury in colorectal surgery
“Splenic injury is a major intraoperative complication of abdominal surgery and places patients at a higher risk of morbidity and mortality, of longer operating time, and of longer hospital stay. Splenic injuries may be managed nonoperatively or by splenorrhaphy, partial splenectomy, or complete splenectomy. Because splenectomy is reported to have higher mortality rates than splenorrhaphy, great effort is taken to preserve the spleen; however, excessive blood loss can mandate splenectomy.”
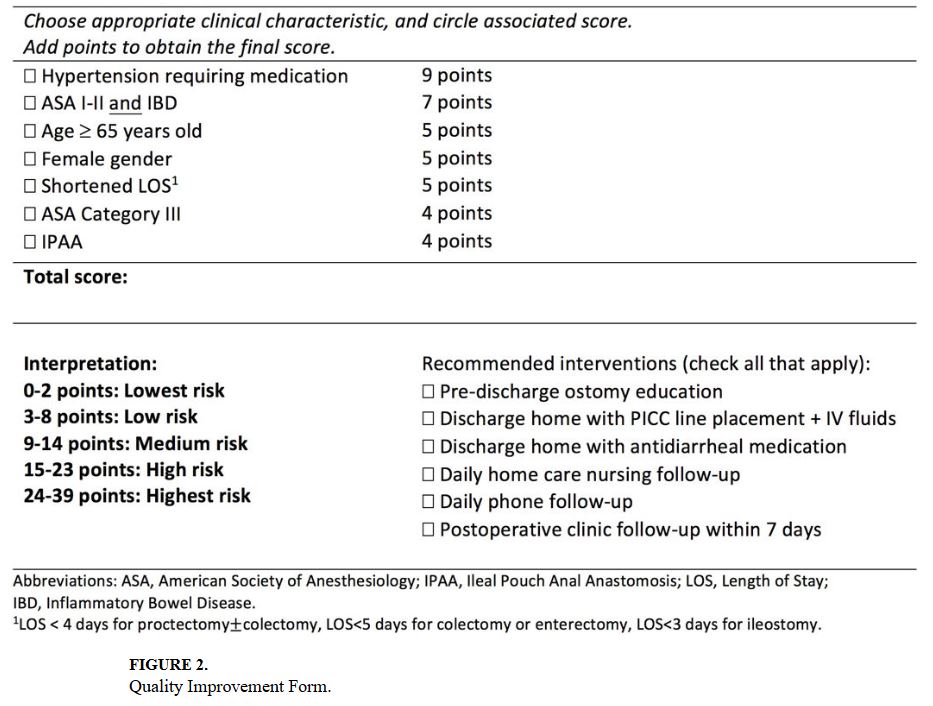
Predicting the Risk of Readmission From Dehydration After Ileostomy Formation
“Readmission within 30-days of hospital discharge has received widespread attention as a
potential healthcare quality indicator. In 2013, the Center for Medicare and Medicaid
Services established the Hospital Readmission Reduction Program (HRRP), a cost-
containment strategy that financially penalizes hospitals with higher than expected 30-day
readmission. Though conditions targeted by the HRRP have been predominately medical, it
is anticipated that readmission after surgical procedures will be used to structure financial
incentives and hospital compensation in the near future.”
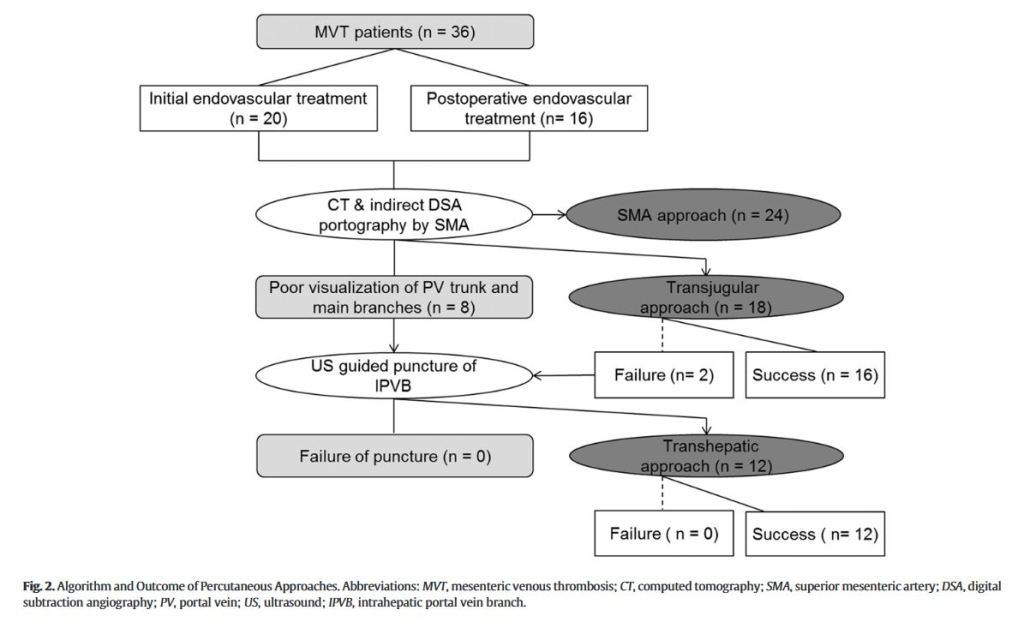
Multidisciplinary Stepwise Management Strategy for Acute Superior Mesenteric Venous Thrombosis
“Acute mesenteric ischemia (AMI) is a rare but catastrophic abdominal vascular emergency associated with a daunting mortality comparable to myocardial infarction or cerebral stroke. Mesenteric vein thrombosis (MVT) is the least common form, accounting for 6% to 9%, of AMI, mainly involving the superior mesenteric vein (SMV). Despite the lack of specific biomarker and insidious symptomatology profile, incidence of acute superior mesenteric venous thrombosis (ASMVT) has been increasing worldwide due to the raised awareness
as well as widespread use of contrast-enhanced computed tomography (CT) portography, which facilitates early diagnosis with sensitivity of over 90%.”