One discussion this week included readmission rates following parathyroidectomy.
References: Ferrandino R, et al. Unplanned 30-day readmissions after parathyroidectomy in patients with chronic kidney disease: a nationwide analysis. Otolaryngology – Head and Neck Surgery. 2017 Dec;157(6):955-965. doi:10.1177/0194599817721154.
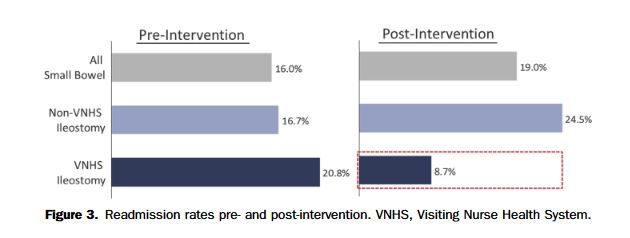
Summary: A retrospective cohort study was performed using the 2013 Nationwide Readmissions Database (NRD) of the Healthcare Cost and Utilization Project (HCUP) from the Agency for Healthcare Research and Quality (AHRQ). In a total of 2756 parathyroidectomies performed in patients with chronic kidney disease, 17.2% had at least one unplanned readmission rate within the first 30-days, and 2.4% had more than one readmission. Overall, readmission rates for chronic kidney disease patients are nearly 5-times that of the general population (Ferrandino et al, 2017).
Hypocalcemia/hungry bone syndrome accounted for 40% of readmissions. While readmissions occurred uniformly throughout the 30 days after discharge, those for hypocalcemia/hungry bone syndrome peaked in the first 10 days and decreased over time.
Weight loss/malnutrition at time of parathyroidectomy and length of stay of 5-6 days conferred increased risk of readmission with adjusted odds ratios of 3.31 and 1.87, respectively. Relative to primary hyperparathyroidism, parathyroidectomies performed for secondary hyperparathyroidism were associated with higher risk of readmission.
The authors conclude: “While there are few patient-specific predictors of readmission, we note that the bulk of these readmissions can be attributed to hypocalcemia. To improve readmission rates after parathyroidectomy in CKD patients, we propose focusing on accurate, appropriate medication reconciliation, and optimizing communication and transitions of care to outside facilities (skilled nursing, dialysis, etc.) to facilitate the comprehensive care of this high-risk patient population” (Ferrandino et al, p.964).
Additional Reading: Sharma J, et al. Improved long-term survival of dialysis patients after near-total parathyroidectomy. Journal of the American College of Surgeons. 2012 Apr;214(4):400-407. doi:10.1016/j.jamcollsurg.2011.12.046.
Westerdahl J, et al. Risk factors for postoperative hypocalcemia after surgery for primary hyperparathyroidism. Archives of Surgery. 2000 Feb;135(2):142-147.