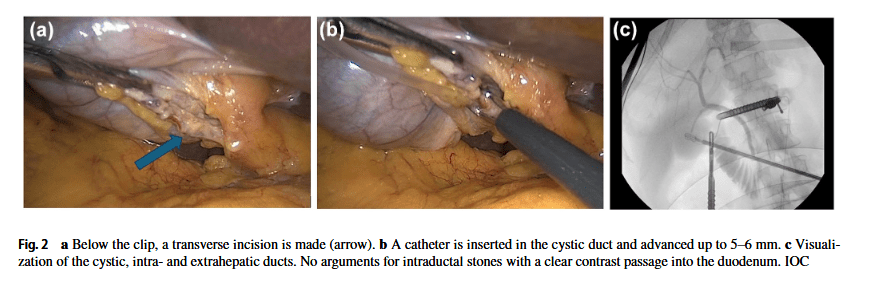
“The role of routine IOC during cholecystectomy has been controversial. Opponents to routine IOC assert that this procedure increases operating times and exposes caregivers and patients to radiation. In addition, there is the possibility of detection of indolent CBD stones with consequently unnecessary removal. On the other hand, advocates in favor
of routine IOC state that intraoperative visualization of the bile duct anatomy may decrease either the rate of complications such as CBD injury, or hospital readmissions for subsequent removal of retained CBD stones. Despite lacking strong evidence for not performing IOC vs. routine IOC vs. selective IOC, fitting in one of these three groups can depend on training, technical experience, and surgical habit. If a surgeon never performs IOC in their daily practice, they are not eager to change their habits, even though literature may suggest otherwise.”