One discussion this week included the clinical and radiographic signs for operation or nonoperation in the setting of adhesive small bowel obstruction (ASBO).
Reference: Kulvatunyou N, et al. A multi-institution prospective observational study of small bowel obstruction: Clinical and computerized tomography predictors of which patients may require early surgery. The Journal of Trauma and Acute Care Surgery. 2015. 79(3);393-398. doi:10.1079/TA.0000000000000759.
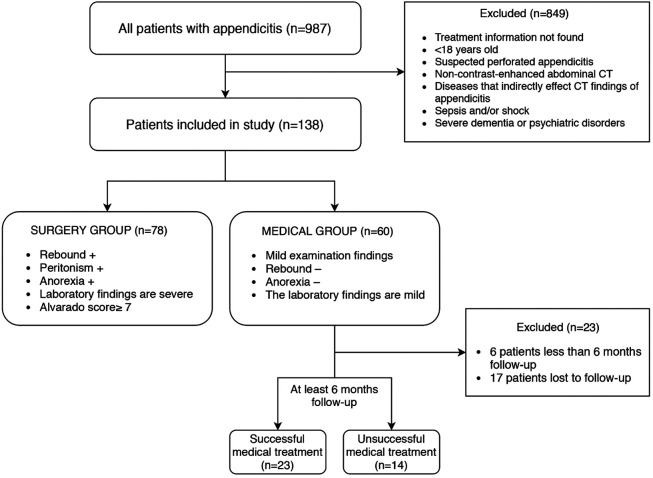
Summary: The absence of flatus and the CT finding of free fluid and high-grade obstruction have been identified by Kulvatunyou et al (2015) as predictors that early operative intervention would be beneficial. This prospective observational study involved 200 patients at three academic and tertiary referral medical centers; 148 in the nonoperative group, 52 in the operative group.
Clinical signs: The only clinical sign identified as a predictor for surgical intervention, “no flatus” was listed in 58% of the operative group, 34% of the nonoperative group. Too large to include here, Table 3 in the text (p.397) lists the univariate analysis of all clinical signs.
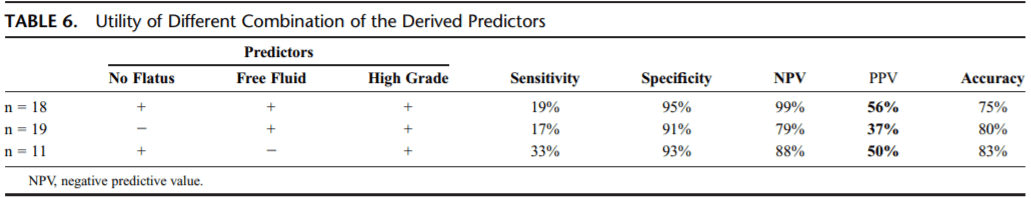
CT findings: Individual CT signs listed include transition point, free fluid, multiple fluid locations, small bowel fecalization, mesenteric edema, closed loop, and high-grad obstruction. All had low PPVs, ranging 21-41%. Using the three predictors identified, the PPV improved but remained low at 37-56% (p.397).
The table below (p.397) illustrates the utility of the three variables in a few combinations.
In the article, the authors state that they are currently (2015) pursuing a study applying the predictors to a different ASBO patient population so as to cross-validate this predictor model. A search for such a study in the published literature was not successful.
Additional Reading: Catena F, et al. Bologna guidelines for diagnosis and management of adhesive small bowel obstruction (ASBO): 2010 evidence-based guidelines of the World Society of Emergency Surgery. World Journal of Emergency Surgery. 2011 Jan 21;6:5. doi: 10.1186/1749-7922-6-5.