Velchev JD, Van Laer L, Luyckx I, Dietz H, Loeys B. Loeys-Dietz Syndrome. Adv Exp Med Biol. 2021;1348:251-264. Full-text for Emory users.
From: Table 11.1. Clinical features at initial diagnosis of LDS. (Velchev JD, et al., p. 253.)
- Vascular findings
- Arterial tortuosity 92%
- Most common in head and neck vessels
- Carotids (55%)
- Vertebral (56%)
- Intracranial (37%)
- Ascending aorta (5%), aortic arch (10%)
- Descending thoracic (4%) or abdominal
- (7%) Ao, also other vessels (e.g. iliacs)
- Most common in head and neck vessels
- Arterial tortuosity 92%
- Aneurysms
- Aorta
- Root 87%
- Ascending 27%
- Arch 10%
- Desc thoracic 15%
- Abdominal 12%
- Vessel beyond Ao 30%
- Aorta

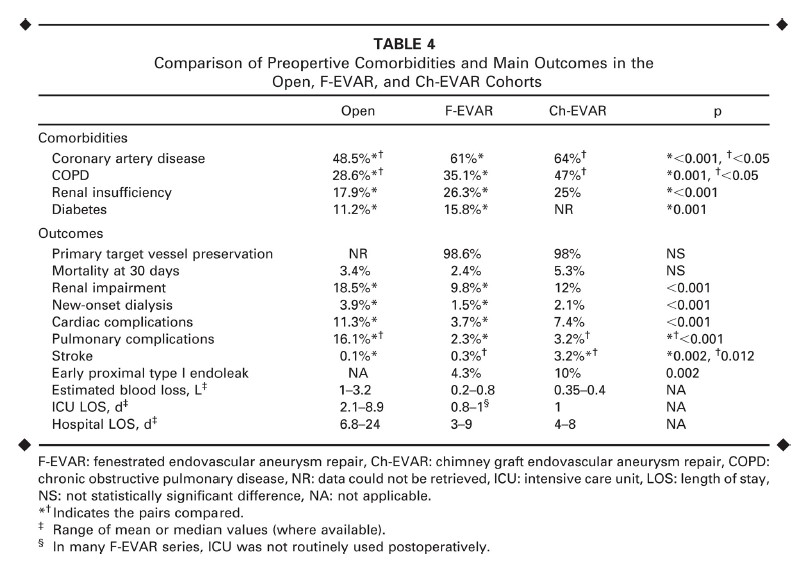
 Click to enlarge.
Click to enlarge.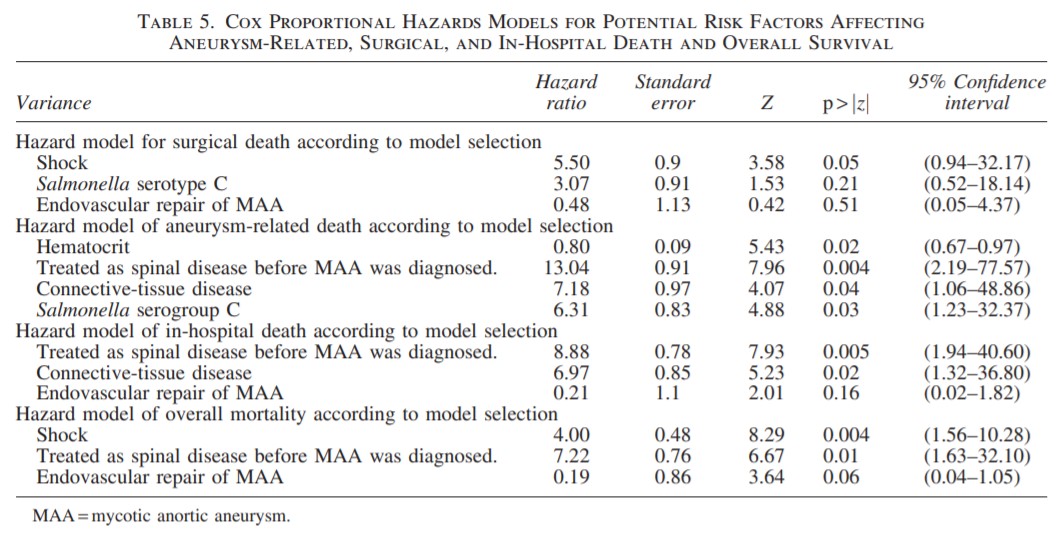 Click to enlarge.
Click to enlarge.